The first two of the features above appear
to reduce the risk of surgery, which is especially important when operating
on patients who suffer from morbid obesity. The fact that there is no
cutting or repositioning of any intestine brings the risk of leak or
obstruction to very low levels (not impossible, as outlined in the risks
section below). The fact that the procedure is almost always done
laparoscopically may allow decreased risk on the vital organs (heart, lungs,
etc.) and may allow quicker recovery in comparison to open procedures
"Removable" in the list of key features
refers to the fact that all surgeons experienced with the Lap-Band report
that it can be removed from the patient with little residual impact on the
stomach. These surgeons report that this is even true when the band has
eroded into the stomach, or become infected, or slipped out of position.
This is possible because the silastic substance from which the band is made
creates essentially no tissue reaction, so that the Band is not stuck in
place over time. This feature also means that the Lap-Band procedure is
"reversible" in a certain sense. The Band could be removed because of
medical necessity, and that if it were not replaced by some other weight
loss procedure that the patient would be guaranteed to experience
significant weight regain.
The feature of the Band that deserves the
most attention is that it is adjustable. This is the feature that makes the
Band (in many published reports) successful in helping patients achieve
significant sustained weight loss. After all, if the Lap-Band were not
successful, then the decrease in operative risk would not mean much. The
fact that the Band can be adjusted to help the patient modify their eating
pattern in a way that is specific to that patient is the feature that makes
it different from the failed VBG, which created a fixed/hard restriction on
eating that frequently led to problems over the long haul.
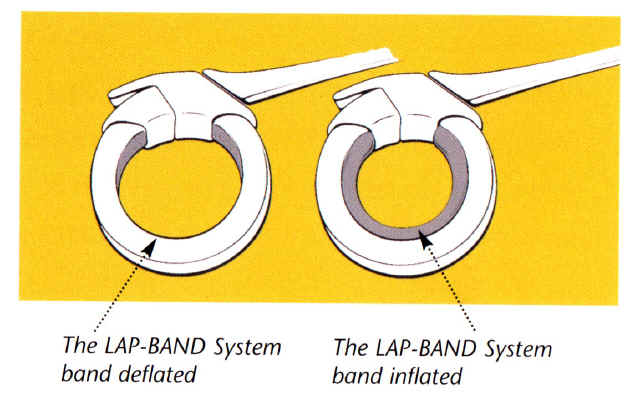
There are several other potential
advantages claimed by advocates of the Lap-Band, which deserve mention.
Slower weight loss - the Lap-Band
aims to create slower and steadier weight loss than the results seen after
most other surgical procedures. Most weight loss operations create very
rapid weight loss in the first few months, which then slows and stabilizes
at 10-18 months after surgery. On the other hand, Lap-Band patients begin
with a relatively loose Band that allows ongoing intake of nutrition, and
the Band is gradually "tightened" according to the patient's weight progress
and satiety symptoms. This approach aims to achieve a weight loss of 1-2
pounds per week, that continues up to or beyond 24 months after surgery.
Lap-Band advocates promote this difference as "gentler" or "safer" or "more
physiologic," but we have frankly seen very few nutritional problems in our
many gastric bypass patients related to rapid weight loss.
Iron, calcium, B12 - operations
that involve rearrangement of the small intestine such as the gastric bypass
or the BPD-DS create a deficiency of absorption of these nutrients. Purely
restrictive procedures such as the Lap-Band should theoretically not cause
such problems because no intestine is bypassed. Caution is needed, however;
almost all VBG patients we see for surgical repair are deficient in Iron
and B12. It may well turn out that the reduction in overall intake is more
important than the specific bowel anatomy. In our practice for the time
being, we are recommending exactly the same supplements after either the
gastric bypass or the Lap-Band.
Open questions The Lap-Band
system has only been in use since the early/mid-1990's, so there is no
long-term data on outcomes. Unbiased observers have raised several
questions about the Lap-Band as outlined below:
Weight loss results & maintenance -
early studies from Europe reported weight loss results that were less
substantial than the Gastric Bypass. However, more recent studies from
Australia (especially from Dr. Paul O'Brien and Dr. George Fielding) have
put out reliable-appearing results in which weight loss after Lap-Band is
essentially equivalent to GBP. The course of weight over many years after
Lap-Band points in the direction of long term maintenance of weight, but the
actual long term results do not yet exist.
Band erosion - all surgeons who
perform the Lap-Band have found erosion of the Band into the patient's
stomach in a small percentage of cases. It appears that this event (which
requires removal of the Band) occurs mainly in the first year or so after
surgery. However the truly long-term incidence of Band erosion remains to
be seen.
Esophageal function - some patients
have experienced failure of normal esophageal peristalsis (swallowing
function) after Lap-Band. If this occurs, it causes painful swallowing,
reflux, or regurgitation. Band deflation or removal is required. More
recent studies suggest that the occurrence of esophageal failure arises from
tightening the Band too aggressively, and that this complication can be
almost completely avoided.
Silastic reaction - it is possible
that the material of the Band could create some type of body immune reaction
that stimulates a separate disease process such as arthritis or Systemic
Lupus Erythematosis (SLE). However the Band is made of a silicone elastomer
which is completely non-reactive to the body tissues, as far as it has been
possible to determine. The same type of material has been in use in a
number of implanted medical devices over time, and no problems with tissue
reaction have been demonstrated. Here again, the early data is reassuring
but no true long-term information exists.
Risks specific to Lap Band
Band erosion - the Band can erode
through the wall of the stomach. This results in loss of restriction to
eating, or Band infection caused by leakage of stomach juices onto the
Band. It is reported that such erosion rarely results in a sudden
life-threatening situation for the patient. Erosion of the Band almost
always requires removal of the Band, with plans for a later conversion to a
different weight loss procedure.
Band slippage or shifting - the
Band must remain in the correct position on the upper stomach in order to
function properly. If it slips out of place or twists, it is likely to
cause obstruction of the stomach, requiring fairly urgent re-operation to
reposition the Band.
Swallowing problems - as mentioned
above, the function of the Band as a partial blockage against outflow from
the stomach pouch may cause the esophagus (which normally pushes food down
in a very coordinated way) to become fatigued or damaged and to fail its
normal swallowing function. The rate of occurrence of this problem varies
widely among published reports, with the more recent studies being more
reassuring.
Hardware breakage - the Band, the
port, and the connection tubing are designed to last for life. In fact, the
Band itself is almost never reported to break or leak. However, the tubing
and the port definitely can become twisted, kinked, or broken. Such events
require re-operations (usually minor) for repair or repositioning of the
problem spot.
Injury to stomach or other nearby organs during surgery - even in
capable hands, the maneuvers involved in placing the Band may sometimes
create injury to the stomach, esophagus, spleen, liver, or to the tissues
involved in placement of the trochars. Sometimes such injuries can be
addressed at the time of surgery and the Band can still be placed.
Sometimes the nature of the injury means it is most reasonable to abandon
the operation.

